This web page was produced as an assignment for Genetics 677, an undergraduate course at UW-Madison.
What is Crohn's Disease?
Crohn's disease is classified as an inflammatory bowel disease (IBD). It is chronic in nature, affecting the gastrointestinal (GI) tract. Though it can occur anywhere throughout the GI tract, it most commonly affects the lower portion of the small intestine and the colon. The associated inflammation damages the intestinal lining, resulting in a range of symptoms including malnutrition, dehydration, diarrhea, and abdominal pain. Over time, the inflammation can result in a swelling of the intestinal wall, leading to blockage. Some patients also develop fistulas, or holes in the intestinal wall, leading to internal infection [1,2,4].
YouTube, 2011. Mayo Clinic. Taken from: http://www.youtube.com/watch?v=fxVemmimuhg&feature=player_embedded
Disease Prevalence
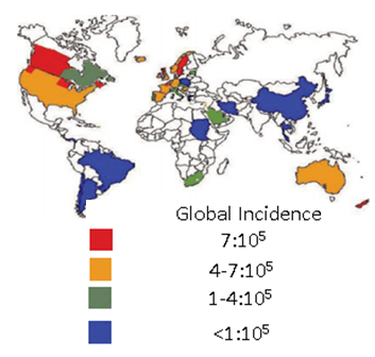
Crohn's disease affects approximately 700,000 people in the United States, with similar rates in Europe and lower rates elsewhere [7]. Disease prevalence is highest in those with Eastern European ancestry and is slightly higher in men than in women. Diagnosis usually occurs in individuals between 15 and 30 years old, although the disease can present itself at any age [3]. Below is a map indicating frequencies of Crohn's Disease by country:
Causes of Crohn's disease
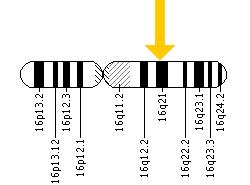
The precise cause of Crohn's disease is unknown, though immune system malfunction, environment, and genetics have been implicated [5]. It is currently thought that inflammation in the lining of the intestine results from the immune system overreacting to foreign particles and from an erroneous response to the intestines' naturally present microbes. Several genes involved in the immune response have been associated with the disease. One such gene is NOD2, located on the 16th chromosome.
The Role of NOD2 in Crohn's Disease
Nucleotide-binding oligomerization domain-containing protein 2 (NOD2) was the first gene to be associated with Crohn's disease [7]. Healthy NOD2 protein responds to the presence of invading bacteria through interactions with muramyl dipeptide (MDP), a component of bacterial cell walls. The response of the NOD2 protein to MDP initiates a biochemical pathway which ultimately leads to increased immune response through the NF-κB transcription factor [6].
Multiple Crohn's disease-associated NOD2 variants have been shown to disrupt this NOD2/MDP interaction. The most common variants are SNP8, SNP12, SNP13, which account for the majority(81%) of NOD2-related Crohn's. SNP8 and SNP12 are missense mutations while SNP13 results in a frameshift causing early truncation of the protein. See the bottom of the protein domains page for a detailed explanation of where these mutations are located. It is believed that such variants fail to initiate immune response to invasive bacteria. The invading bacteria can then inhabit the intestinal lining and cause the harmful inflammation associated with the disease. Mutations in NOD2 in mice have also been found which are hyper-responsive to MDP, suggesting the possibility that such mutants would over-activate the immune system, again resulting in inflammation of the intestine [6]
Multiple Crohn's disease-associated NOD2 variants have been shown to disrupt this NOD2/MDP interaction. The most common variants are SNP8, SNP12, SNP13, which account for the majority(81%) of NOD2-related Crohn's. SNP8 and SNP12 are missense mutations while SNP13 results in a frameshift causing early truncation of the protein. See the bottom of the protein domains page for a detailed explanation of where these mutations are located. It is believed that such variants fail to initiate immune response to invasive bacteria. The invading bacteria can then inhabit the intestinal lining and cause the harmful inflammation associated with the disease. Mutations in NOD2 in mice have also been found which are hyper-responsive to MDP, suggesting the possibility that such mutants would over-activate the immune system, again resulting in inflammation of the intestine [6]
Treatments for Crohn's Disease
Currently there is no true cure for Crohn's but there are many treatments which alleviate the symptoms. Aminosalicylates and Biologics are used to downregulate inflammation. Such drugs are often quite effective but come with side effects such as excessive bleeding, immune deficit, and depression. Antibiotics are often used to treat the infected sites which result from the disease, but they fail to control the disease itself. Immune suppressors and Steroids are also used to lessen inflammation, but again these are treating only symptoms and not the disease itself. Also, such treatments can lead to patients being more susceptible to infection [8]. Research into understanding and curing Crohn's Disease is ongoing. If you would like to donate towards this research please visit the Crohn's & Colitis Foundation of America.
References
[1] "CCFA.org: About Crohn's Disease." CCFA.org: Home. Web. <http://www.ccfa.org/info/about/crohns>.
[2] Chiodini, RJ. "Crohn's Disease and the Mycobacterioses: A Review and Comparison of Two Disease Entitie." Ameican Society for Microbiology 2 (1989): 90-117. Print.
[3] "Crohn's Disease - Causes, Symptoms & Treatment." EMedicineHealth.com. Web. <http://www.emedicinehealth.com/crohn_disease/article_em.htm>.
[4] "Crohn's Disease Symptoms." Tree. Web. <http://www.tree.com/health/crohns-disease-symptoms.aspx>.
[5] Staff, Mayo Clinic. "Crohn's Disease: Causes - MayoClinic.com." Mayo Clinic. Web. <http://www.mayoclinic.com/health/crohns-disease/DS00104/DSECTION=causes>.
[6] Vignal, Cecile, Elisabeth Singer, Laurent Peyrin-Biroulet, Pierre Desreumaux, and Mathias Chamaillard. "How NOD2 Mutations Predispose to Crohn's Disease?" Microbes and Infection 9.5 (2007): 658-63. Print.
[7] Yazdanyar, Shiva, Maren Weischer, and Borge G. Nordestgaard. "Genotyping for NOD2 Genetic Variants and Crohn Disease: A Metaanalysis." Clinical Chemistry 55.11 (2009): 1950-957. Print.
[8] "Treatment for Crohn's Disease - WebMD." WebMD. WebMD. Web. <http://www.webmd.com/ibd-crohns-disease/crohns-disease/tc/crohns-disease-treatment-overview>.
[9] Banner Image adapted from: Kosiewicz MM, Nast CC, Krishnan A, et al. Th1-type responses mediate spontaneous ileitis in a novel murine model of Crohn's disease. J Clin Invest. 2001;107(6):695-702.
[2] Chiodini, RJ. "Crohn's Disease and the Mycobacterioses: A Review and Comparison of Two Disease Entitie." Ameican Society for Microbiology 2 (1989): 90-117. Print.
[3] "Crohn's Disease - Causes, Symptoms & Treatment." EMedicineHealth.com. Web. <http://www.emedicinehealth.com/crohn_disease/article_em.htm>.
[4] "Crohn's Disease Symptoms." Tree. Web. <http://www.tree.com/health/crohns-disease-symptoms.aspx>.
[5] Staff, Mayo Clinic. "Crohn's Disease: Causes - MayoClinic.com." Mayo Clinic. Web. <http://www.mayoclinic.com/health/crohns-disease/DS00104/DSECTION=causes>.
[6] Vignal, Cecile, Elisabeth Singer, Laurent Peyrin-Biroulet, Pierre Desreumaux, and Mathias Chamaillard. "How NOD2 Mutations Predispose to Crohn's Disease?" Microbes and Infection 9.5 (2007): 658-63. Print.
[7] Yazdanyar, Shiva, Maren Weischer, and Borge G. Nordestgaard. "Genotyping for NOD2 Genetic Variants and Crohn Disease: A Metaanalysis." Clinical Chemistry 55.11 (2009): 1950-957. Print.
[8] "Treatment for Crohn's Disease - WebMD." WebMD. WebMD. Web. <http://www.webmd.com/ibd-crohns-disease/crohns-disease/tc/crohns-disease-treatment-overview>.
[9] Banner Image adapted from: Kosiewicz MM, Nast CC, Krishnan A, et al. Th1-type responses mediate spontaneous ileitis in a novel murine model of Crohn's disease. J Clin Invest. 2001;107(6):695-702.
Created by: Jonathan M. Peterson
[email protected]
Genetics 677 Assignment, Spring 2012
Last Update: 5/20/2012
[email protected]
Genetics 677 Assignment, Spring 2012
Last Update: 5/20/2012